The queue began forming before sunrise. By the time the gates of the Nkosi Johnson Community Health Centre opened at 7:30 a.m., nearly 200 people had gathered — young women in school uniforms, men in work overalls, grandmothers clutching worn handbags, and teenagers who had skipped breakfast to be first in line. They were not here for food parcels or social grants. They were here for something far more precious: a shot of hope.
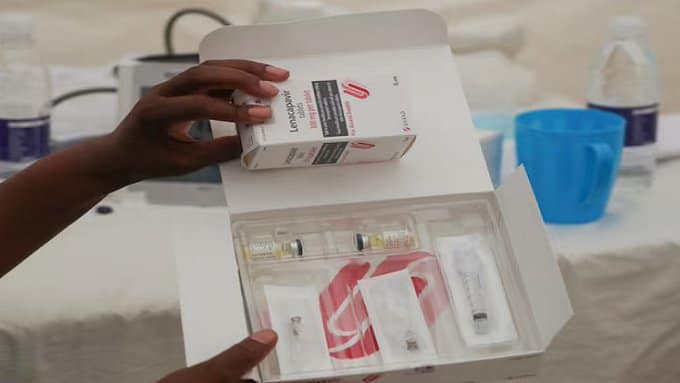
On a crisp autumn morning in Mpumalanga, South Africa received its first shipment of Lenacapavir — a groundbreaking twice-yearly HIV prevention injection that offers long-lasting protection against the virus with just two doses a year. The arrival of the first vials at the Mbombela District Pharmaceutical Depot was low-key, almost clinical: a white delivery truck, two security escorts, a clipboard, and a signature. But the moment the temperature-controlled boxes were wheeled into the storage facility, a small crowd of health workers broke into spontaneous applause.
For a province that has long carried the heaviest burden of the world’s most severe HIV epidemic, the arrival of Lenacapavir is nothing short of revolutionary.
A breakthrough decades in the making
Lenacapavir, developed by US-based pharmaceutical giant Gilead Sciences, represents the most significant advancement in HIV prevention since the introduction of daily oral pre-exposure prophylaxis (PrEP) in 2012. Unlike daily pills, which require strict adherence and can be stigmatizing for users who fear being seen taking medication, Lenacapavir is administered subcutaneously twice a year — a convenience that could transform HIV prevention, particularly among young women and other high-risk populations.
Clinical trials published in The New England Journal of Medicine in 2024 showed that Lenacapavir reduced the risk of HIV infection by 96% among participants who received the injection every six months. Crucially, adherence rates in the trial exceeded 90% — a dramatic improvement over daily PrEP, where real-world adherence often falls below 50% due to pill fatigue, side effects, and social pressures.
“Daily PrEP changed the game when it arrived,” said Dr. Nomsa Mahlangu, head of HIV prevention programs at the Mpumalanga Department of Health, speaking at a small media briefing at the depot. “But Lenacapavir changes the sport entirely. Two injections a year. That’s it. No daily reminder. No pill bottle to hide. No pharmacy run every month. For young women who face violence if a partner discovers they are protecting themselves — this could be the difference between life and death.”
Mpumalanga: Ground zero of the epidemic
The choice of Mpumalanga as the first recipient of Lenacapavir was not accidental. According to the Human Sciences Research Council’s latest household survey, Mpumalanga has the highest HIV prevalence of any province in South Africa, with an estimated 17.4% of the adult population living with the virus. Among young women aged 15 to 24, prevalence exceeds 20% in several districts.
For years, prevention efforts here have struggled against a perfect storm of poverty, gender-based violence, migrant labor patterns, and limited access to healthcare. The province’s network of mines draws thousands of workers from across southern Africa, creating conditions that facilitate rapid transmission. Rural clinics are often understaffed. And stigma remains a formidable barrier: many young people fear being seen collecting PrEP pills or condoms, fearing gossip or accusations of promiscuity.
“The injection solves so many of those problems at once,” said Thabo Nkosi, a community health worker who has spent 15 years doing door-to-door HIV education in the township of KaNyamazane. “You come to the clinic twice a year. You don’t leave with a bag of pills. Nobody knows why you were here unless you tell them. For a young woman who is sexually active but not ready to tell her family — that is freedom.”
The first recipients: ‘I feel like I can breathe’
By mid-morning, the first doses had been administered. At the front of the line was Lerato Mkhabela, 22, a second-year education student at the University of Mpumalanga. She had learned about Lenacapavir from a WhatsApp message forwarded by a friend the night before. By 5 a.m., she was outside the clinic.
“I was using the daily pill for two years,” Lerato said, rolling up her sleeve as a nurse prepared the injection. “But I would forget. Or I would be too scared to take it in front of my boyfriend. He doesn’t know I’m on PrEP. He would think I’m cheating or that I think he has something. It was exhausting, always hiding.”
The injection itself took less than thirty seconds. Lerato winced briefly, then smiled. “That’s it?” she asked. The nurse nodded. “Come back in six months.”
Outside, Lerato sat on a concrete bench, rubbing her arm. “I feel like I can breathe,” she said. “Two times a year. I can do that. I can plan for that. My future just got a lot bigger.”
Behind her, 19-year-old Sipho Dlamini, a part-time taxi assistant, waited for his turn. “People think HIV is a ‘girl disease’ or a ‘gay disease,'” he said, shaking his head. “That’s how people get sick. I’m here because I want to live. Simple. This injection makes it easy to be responsible. No excuses now.”
The rollout: Challenges ahead
Despite the euphoria, health officials were quick to temper expectations with realism. The first shipment of Lenacapavir is small — just 5,000 doses, enough for 2,500 people for one year. The national target is to reach 100,000 people by the end of 2026, but that will require massive investment in cold chain logistics, healthcare worker training, and community mobilization.
Lenacapavir must be stored at temperatures between 2°C and 8°C — a significant challenge in a province where summer temperatures often exceed 35°C and where some remote clinics still experience intermittent electricity supply. The Mpumalanga Department of Health has deployed solar-powered refrigeration units to 28 priority clinics, but officials acknowledge that gaps remain.
“The science is ready. The question is whether our systems are ready,” said Dr. Mahlangu. “We cannot afford to waste a single dose. Every vial represents hope for someone. We will move slowly at first, then accelerate. But we will not rush and risk failure.”
Cost is another barrier. While Gilead Sciences has agreed to a tiered pricing model for low- and middle-income countries, the annual cost per patient is still expected to be around $120 (approximately R2,200) — significantly higher than daily PrEP, which costs as little as $60 per year. The South African government has committed R400 million to the initial rollout, but civil society groups warn that sustained funding will require donor support.
“It is expensive,” acknowledged Sibongile Tshabalala, director of the Mpumalanga AIDS Council. “But what is the cost of doing nothing? New infections cost the health system billions every year. Prevention is always cheaper than treatment. Always.”
A turning point in the 40-year war
Since the first cases of HIV were recognized in 1981, the world has lost an estimated 40 million people to AIDS-related illnesses. South Africa, with the largest treatment program on the planet, has brought the epidemic under control — but not under submission. Every week, approximately 1,500 South Africans are newly infected. Young women account for nearly half of those infections.
Lenacapavir is not a cure. It does not treat people already living with HIV. It is a prevention tool — and one that arrives at a moment when global attention on HIV has faded, displaced by COVID-19, mpox, and other emerging threats. But for the women queuing outside the Nkosi Johnson Clinic, the global headlines matter less than the needle about to enter their arms.
“My mother died of AIDS in 2010,” said Gloria Mthimkulu, 34, a mother of three who was among the first to receive the injection. “I was 18. I watched her waste away. I swore then that I would not die like that. I have used condoms. I have used pills. Now I have this. Two times a year. My children will grow up with a mother. That is all I have ever wanted.”
The road ahead
Over the next six months, Lenacapavir will be rolled out to an additional 12 districts in Mpumalanga, followed by targeted distribution in KwaZulu-Natal, Gauteng, and the Eastern Cape — the other high-burden provinces. The National Department of Health has launched a multimedia awareness campaign, featuring radio ads in isiZulu, Sesotho, and Xitsonga, as well as social media influencers promoting the “Twice-a-Year Defense.”
But the real campaign will happen in places like this: in clinic waiting rooms, on taxi rank benches, in church halls, and over kitchen tables. It will happen when one friend tells another. When a grandmother brings her granddaughter. When a young man decides that protecting himself is not weakness but strength.
As the sun set over Mbombela, the queue outside the Nkosi Johnson Clinic had finally dwindled. By day’s end, 187 people had received the first dose of Lenacapavir. One hundred and eighty-seven stories of hope, each one a small victory in a war that has claimed too many.
Nurse Sibongile Masilela, who administered the final injection of the day, sat down on a plastic chair and exhaled. She has been an HIV nurse for 22 years. She has held the hands of dying patients. She has told hundreds of young people that their lives have changed forever. But today, she said, was different.
“Usually, I am giving bad news or managing sickness,” she said, wiping her eyes. “Today, I gave prevention. I gave a future. I gave a young girl the chance to grow old. That is why I became a nurse. That is why I stayed. Today, I remembered why.”
The Lenacapavir vial she used is now empty. But the hope it carried — that is just beginning to flow.
A new chapter
South Africa has been here before: at the dawn of a new technology that promises to bend the curve. Antiretrovirals in the early 2000s. Prevention of mother-to-child transmission. Medical male circumcision. Daily PrEP. Each breakthrough was met with excitement, then the sobering work of implementation.
Lenacapavir will be no different. The vials must be kept cold. The nurses must be trained. The communities must be reached. The funding must be sustained. But for one day, in one province, none of that seemed to matter.
What mattered was the queue. The needle. The small scar that will fade. And the knowledge that for the next six months, nearly 200 people in Mpumalanga will walk through the world protected — not by fear, not by shame, but by science.
The fight against HIV is not over. But for the first time in a long time, it feels like the finish line might actually be visible. And in Mpumalanga, they are already running toward it.